

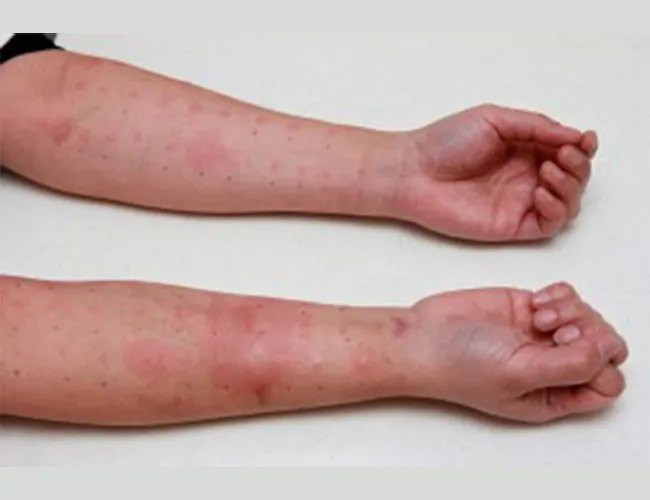
A severe allergic reaction is called anaphylaxis and can be potentially life threatening. Typically, during anaphylaxis, several areas of the body are affected, which can cause breathing difficulties and requires immediate medical attention.

Milk, eggs, soy, wheat, peanuts, tree nuts, fish, and shellfish are among the most common foods that cause allergies. A child could be allergic to many other foods. However, 90% of all reactions in children occur from these these eight common allergens:
Children who are allergic to milk, eggs, soy, and wheat often outgrow the allergy, while outgrowing a nut or seafood allergy is far less common. Breastfed infants can experience an allergic reaction to a food ingested by the mother.
In order to confirm a food allergy, your doctor will most likely recommend additional testing which may include:
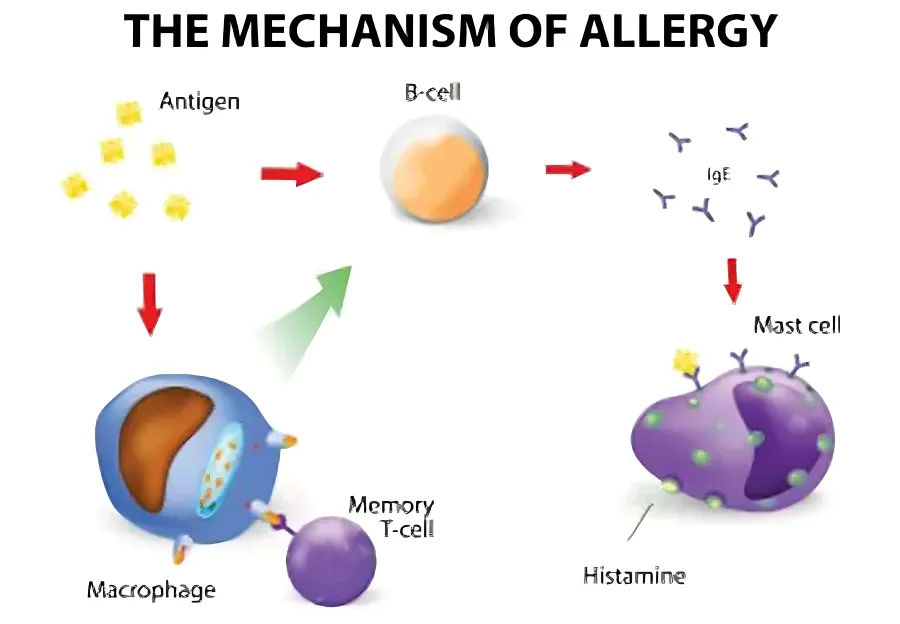
Treating a food allergy usually involves avoiding the foods that contain the allergen causing the reaction. There is not a cure for food allergies. Milder symptoms can be treated with:
Managing your child’s food allergy involves not only avoiding certain foods, but also keeping others informed of foods that your child cannot have. A successful management plan includes:

Symptoms of a food allergy can range from extremely mild to life threatening. Allergic reactions can affect the gastrointestinal tract. More severe gastrointestinal symptoms like difficulty swallowing (dysphagia) and heartburn that is unresponsive to antireflux therapy has become increasingly recognized as Eosinophilic Esophagitis (EoE). EoE is an inflammatory disorder characterized by the deposition of eosinophils in the wall of the esophagus. The esophagus is normally devoid of any eosinophils. Gastroesophageal reflux disease can induce a mild eosinophilia response but severe eosinophilic infiltration of the esophagus is presumably due to allergic causes. Eosinophilic esophagitis affects both children and adults. For unknown reasons, males are more commonly affected than females. People with EoE commonly have other allergic diseases such as asthma or eczema but a personal or family history of other allergic diseases may also be absent.
In children, symptoms of EoE include feeding disorders, vomiting, abdominal pain, difficulty swallowing, and food impaction. The major symptoms among adults with EoE are difficulty swallowing solid food, food impaction, heartburn, and chest pain. The exact pathogenesis of EoE is unknown.
Upper GI endoscopy (EGD-Esophagogastroduodenoscopy) with mucosal biopsies is required to make the diagnosis of EoE. Biopsies reveal an increased number of eosinophils (>20 cells per high powered field) in the squamous epithelium.
Treatment for EoE includes dietary changes and steroids that are recommended by the physician on a case-by-case basis. The natural history of EoE is unknown but no cases of cancer have been reported to date.
The diagnosis of EoE is often delayed because of the lack of awareness of this disorder. The importance of recognizing this condition lies in the fact that EoE requires therapeutic measures different than those used for gastroesophageal reflux. Please consult with your physician if you are concerned that you or a family member may have symptoms consistent with eosinophilic esophagitis.
Food intolerance is often confused with a food allergy due to the similarity in symptoms. While food intolerance can be uncomfortable, it does not involve the immune system and is rarely dangerous. Children with food intolerance can experience symptoms such as: