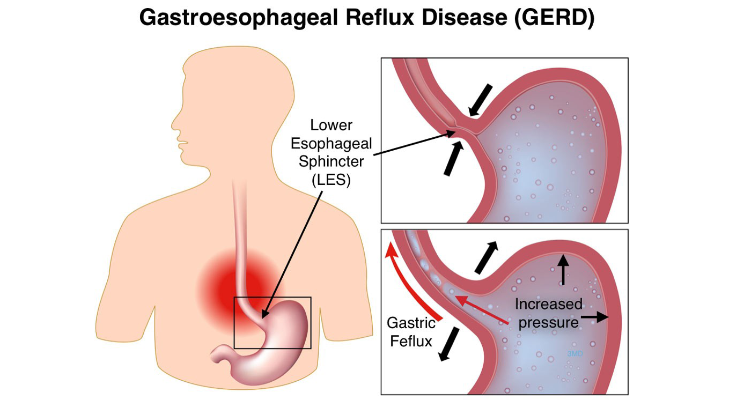
Gastroesophageal reflux disease (GERD) in children is a digestive disorder in which the gastric acid from the stomach moves upward into the esophagus. Most people have gastric acid reflux occasionally; however, if reflux is occurring frequently, it can develop into GERD. Gastroesophageal reflux (GER) is the result of a malfunctioning valve at the end of the esophagus. This lower esophageal sphincter (LES) muscle normally opens and closes to allow food into the stomach. If the muscle opens, or relaxes, longer or more often than it should, stomach acid refluxes into the esophagus. This reflux can cause heartburn or vomiting. If reflux enters the throat (i.e., trachea or wind pipe), it is referred to as laryngopharyngeal reflux, which results in throat clearing, throat pain, coughing, and chest congestion. GER is a common occurrence in infants, with more than 50% of children three months or younger having at least one vomiting episode per day. The majority of babies outgrow GER by age one due to increased muscle control. Older children who are experiencing GER need to be evaluated by a doctor to determine the cause of the problem and receive treatment.
What Causes GERD?
Causes of GERD in children are typically different than the causes for infants or adults. Anything that increases pressure below the LES can contribute to a child having GERD, including:
- Overeating
- Obesity
- Constipation
- Medication (some antihistamines, pain medicines, and antidepressants can contribute)
- Secondhand smoke
Certain foods that can affect the functionality of the LES can contribute to GER:
- Peppermint
- Foods high in fat
- Acidic foods, such as citrus (lemons, limes, oranges), tomatoes, and tomato sauces
- Chocolate
- Carbonated beverages and caffeine
Common Symptoms
Heartburn is the most common symptom of GERD in adults, but children may or may not experience heartburn. When they do, they often have difficulty describing the sensation. Children with GERD typically complain of tummy pain or chest discomfort, most frequently after meals. Common symptoms of GERD include digestive and pulmonary symptoms:
- Frequent vomiting
- Excessive burping
- Refusal to eat or gagging during eating
- Weight loss
- Poor appetite
- Bad breathe (halitosis)
- Cavities or breakdown of tooth enamel
- Persistent cough or throat clearing (caused by secretions of the larynx, or voice box)
- Sore throat, pain with swallowing (dysphagia - caused by recurrent tonsil infection)
- Hoarseness (dysphonia)
- Breathing problems, wheezing or congestion
- Frequent upper respiratory or ear infections
How to Treat It
If your child is an infant, treatment will generally be focused on lessening symptoms, as the underlying problem typically resolves itself in time. Some successful measures used to reduce symptoms are:
- Elevating the head of the child's crib
- Thickening the baby's milk or formula with rice cereal or thickening agents (only with doctor's recommendation)
- Holding the baby upright after feedings for 30 minutes
- Introducing solid foods (only with doctor's recommendation)
Treatment for older children experiencing GERD includes similar measures, as well as lifestyle and dietary changes and possibly medication. Common treatments include:
- Raising the head of the child's bed
- Eating small, more frequent meals instead of three larger meals per day
- Remaining upright for 2-3 hours after eating
- Regular exercise
- Avoiding foods that may aggravate symptoms, such as carbonated beverages, citrus, caffeine, chocolate, and fried or spicy foods
- Medication (your doctor may prescribe a medication for your child or recommend an over-the-counter medicine in order to decrease intestinal gas or neutralize stomach acid; consult your doctor before giving your child any over-the-counter medications for GERD)
If you are concerned that your child may have GERD or is experiencing symptoms of GERD, please set up an
appointment with our office. If you would like more information about gastrointestinal (GI) digestive disorders and nutrition in children, please contact Dr. Mona Dave's
Frisco Office or
Request Appointment Here.
 Gastroesophageal reflux disease (GERD) in children is a digestive disorder in which the gastric acid from the stomach moves upward into the esophagus. Most people have gastric acid reflux occasionally; however, if reflux is occurring frequently, it can develop into GERD. Gastroesophageal reflux (GER) is the result of a malfunctioning valve at the end of the esophagus. This lower esophageal sphincter (LES) muscle normally opens and closes to allow food into the stomach. If the muscle opens, or relaxes, longer or more often than it should, stomach acid refluxes into the esophagus. This reflux can cause heartburn or vomiting. If reflux enters the throat (i.e., trachea or wind pipe), it is referred to as laryngopharyngeal reflux, which results in throat clearing, throat pain, coughing, and chest congestion. GER is a common occurrence in infants, with more than 50% of children three months or younger having at least one vomiting episode per day. The majority of babies outgrow GER by age one due to increased muscle control. Older children who are experiencing GER need to be evaluated by a doctor to determine the cause of the problem and receive treatment.
Gastroesophageal reflux disease (GERD) in children is a digestive disorder in which the gastric acid from the stomach moves upward into the esophagus. Most people have gastric acid reflux occasionally; however, if reflux is occurring frequently, it can develop into GERD. Gastroesophageal reflux (GER) is the result of a malfunctioning valve at the end of the esophagus. This lower esophageal sphincter (LES) muscle normally opens and closes to allow food into the stomach. If the muscle opens, or relaxes, longer or more often than it should, stomach acid refluxes into the esophagus. This reflux can cause heartburn or vomiting. If reflux enters the throat (i.e., trachea or wind pipe), it is referred to as laryngopharyngeal reflux, which results in throat clearing, throat pain, coughing, and chest congestion. GER is a common occurrence in infants, with more than 50% of children three months or younger having at least one vomiting episode per day. The majority of babies outgrow GER by age one due to increased muscle control. Older children who are experiencing GER need to be evaluated by a doctor to determine the cause of the problem and receive treatment. 






