

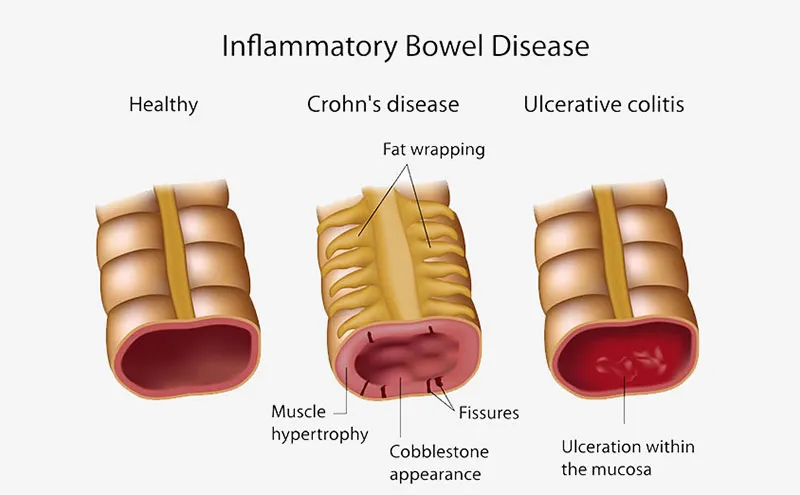
Ulcerative colitis (UC) is an inflammatory bowel disease (IBD) in which the lining of the large intestine (colon) becomes inflamed and sores called ulcers develop which produce mucus and pus. Ulcerative colitis occurs when the body’s immune system mistakes food and other necessary materials in the intestine for invading substances. The immune system then sends white blood cells into the intestinal lining causing inflammation and ulcerations.
Ulcerative colitis is different from Crohn’s disease in that UC affects the colon and the lining of the colon while Crohn’s can affect any part of the gastrointestinal (GI) tract and all layers of the bowel wall.
Symptoms of ulcerative colitis typically develop over time, but can appear suddenly and progress quickly in some cases. Your child may experience symptoms ranging from mild to severe without any obvious reason. Symptoms of ulcerative colitis include:
Children with ulcerative colitis tend to have time periods where symptoms subside and then later flare up. These remission periods can last months or even years, but symptoms do return eventually.
Ulcerative colitis does not have a known cause, however research suggests a combination of factors:
Many scientists believe that patients with UC have an abnormal interaction between an infection and the body’s immune system. In this process, inflammation, which is normally produced temporarily to fight the infection, continues even after the infection has cleared. Approximately 1.4 million Americans are affected by inflammatory bowel disease, with 100,000 being children. Risk factors for UC include:
Complications of Ulcerative Colitis in Children
Complications of ulcerative colitis can arise not only from the condition itself, but also from insufficient nutritional intake. Children with UC can have difficulty getting and absorbing enough calories for proper development. Complications may include:
Ulcerative colitis symptoms can vary depending on the age of your child and the location and severity of inflammation. Your doctor will likely want to collect extensive information about your child, so being well prepared for your appointment will ensure that it goes smoothly. Helpful steps you can take include:
At your appointment, your doctor will perform a thorough examination and review your child’s medical history. Diagnostic testing to confirm a diagnosis may include:
The type of ulcerative colitis diagnosed depends on how much of your child’s colon is affected. The condition can range from mild to severe:
Ulcerative proctitis: The mildest type of ulcerative colitis in which inflammation is limited to the rectum, usually less than 6 inches.
Distal colitis (left sided): Areas of inflammation include the rectum extending as far as the splenic flexure (a sharp bend in the colon near the spleen).
Proctosigmoiditis: Areas of inflammation include the rectum and sigmoid colon (the portion of the colon just above the rectum).
Pancolitis: The entire colon is affected by inflammation.
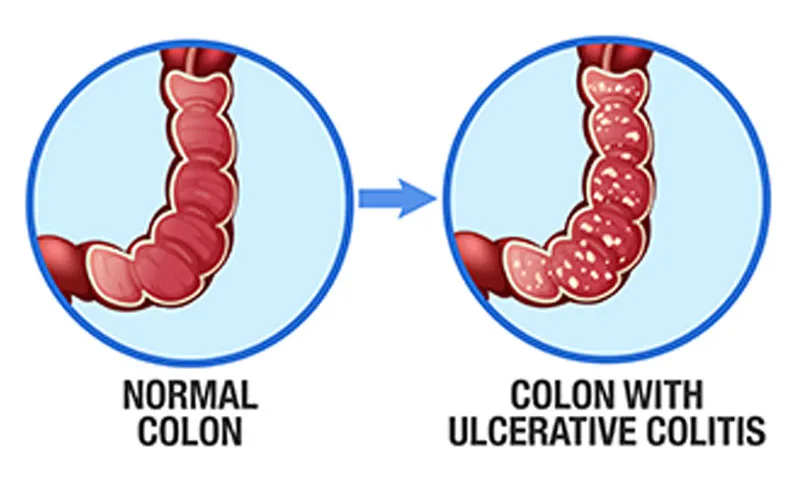
Treating ulcerative colitis involves regulating the immune system in order to control symptoms. With a proper combination of therapies, children with UC can experience a great reduction in symptoms and often long term remission. Goals of UC treatment:
Treatment will depend on what type of UC your child is diagnosed with and how severe the symptoms are. The type of ulcerative colitis diagnosed depends on how much of your child’s colon is affected. The condition can range from mild to severe. Medications that have been successfully used to treat symptoms are:
If your child is diagnosed with ulcerative colitis, you can make dietary and other lifestyle adjustments to help alleviate symptoms:
If you would like more information about gastrointestinal (GI) digestive disorders and nutrition in children, please contact us here.